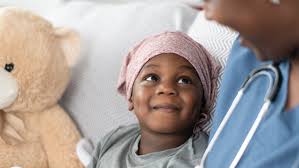
Pediatric oncology is not just about treating cancer in children; it is also about nurturing their emotional and psychological well-being. The journey through cancer treatment can be overwhelming for young patients, often accompanied by fear, uncertainty, and distress. Families, too, face immense emotional challenges, balancing the needs of the sick child with daily life and responsibilities. Recognising the importance of mental and emotional care alongside medical treatment is essential for improving outcomes and ensuring a holistic approach to paediatric oncology.
Understanding the Emotional Impact of Pediatric Cancer
A diagnosis of cancer in a child is life-changing for both the patient and their family. Children may experience anxiety, depression, and behavioural changes, while parents and siblings often confront feelings of helplessness, guilt, and grief. These emotional responses are natural but, if left unaddressed, can affect the child’s overall well-being and ability to cope with treatment.
Early intervention with emotional and psychological support can significantly reduce stress and anxiety. Counselling, play therapy, and structured psychological programmes help children express their feelings safely, understand their treatment, and develop coping mechanisms. By providing these support systems, hospitals can foster resilience and a sense of normalcy, even during prolonged treatment periods.
Role of Specialised Pediatric Oncology Teams
Effective care in pediatric oncology extends beyond medical expertise. Dedicated multidisciplinary teams, comprising paediatric oncologists, psychologists, child life specialists, and social workers, work collaboratively to address the unique needs of each child. These professionals not only oversee medical treatment but also provide continuous emotional support, helping children manage fear, pain, and uncertainty associated with hospital visits and procedures.
Child life specialists, in particular, play a vital role. They use age-appropriate education, play therapy, and interactive activities to help children understand their diagnosis and treatment. This approach reduces anxiety, improves cooperation during procedures, and enhances the overall hospital experience.
Family-Centered Psychological Support
Families are integral to a child’s recovery journey. Hospitals offering comprehensive pediatric oncology care emphasise family-centered support, providing parents and caregivers with counselling and resources to cope with the emotional challenges of cancer care. Support groups allow families to connect with others facing similar experiences, fostering understanding, empathy, and shared strategies for managing stress.
Moreover, guidance from healthcare professionals helps families communicate effectively with the child about their illness, treatment plan, and anticipated outcomes. Such open communication reduces fear and confusion, enabling families to provide consistent emotional reassurance.
Integration of Therapeutic Interventions
Several therapeutic interventions have proven effective in supporting the emotional health of children undergoing oncology treatment. Cognitive-behavioural therapy (CBT), art therapy, music therapy, and mindfulness techniques help children manage anxiety, depression, and pain perception. These interventions complement medical treatment by enhancing coping skills, boosting mood, and improving treatment adherence.
Hospitals that integrate these interventions into routine pediatric oncology care create a supportive environment that nurtures mental and emotional resilience. By addressing the psychological needs alongside physical treatment, children experience better overall outcomes and a more positive hospital experience.
Importance of Educational and Recreational Programs
Maintaining a sense of normalcy is crucial for children in pediatric oncology care. Educational support and recreational activities can prevent feelings of isolation and help maintain developmental progress during treatment. Hospital-based schooling programmes ensure continuity in learning, while recreational activities provide opportunities for social interaction, creative expression, and stress relief.
These programmes not only support the child’s emotional well-being but also empower them to remain engaged in life beyond the hospital setting. By balancing treatment with structured educational and recreational activities, hospitals can significantly improve the quality of life for pediatric patients.
Long-Term Psychological Care
The emotional challenges faced during treatment often extend beyond the hospital stay. Survivors of pediatric cancer may experience ongoing anxiety, post-traumatic stress, or adjustment difficulties. Long-term psychological support, including periodic counselling, peer support groups, and follow-up therapy, ensures that children and their families continue to receive guidance and reassurance.
Hospitals providing pediatric oncology care recognise that recovery is a lifelong process. By offering sustained emotional and psychological support, they help survivors reintegrate into school, social settings, and everyday life, promoting holistic recovery and long-term well-being.
Conclusion
In pediatric oncology, treating the disease is only one part of the healing process. Emotional and psychological support is equally crucial for children and their families, helping them manage the challenges of cancer treatment with resilience and hope. Hospitals that adopt a multidisciplinary, family-centered approach, integrating therapeutic, educational, and recreational interventions, create an environment where young patients can thrive despite the challenges of their illness.
By prioritising emotional well-being alongside medical treatment, pediatric oncology centres can foster better coping mechanisms, improve treatment adherence, and ultimately enhance the quality of life for children battling cancer. Comprehensive support ensures that families feel guided and supported at every step, making the journey through pediatric oncology more manageable, compassionate, and hopeful.